AI Podcast Generator vs Assured
Side-by-side comparison to help you choose the right AI tool.
AI Podcast Generator
AI Podcast Generator is an AI-powered platform that transforms text, articles, or ideas into natural-sounding podcast.
Assured
NCQA-certified: Fast provider enrollment.
Visual Comparison
AI Podcast Generator
Assured
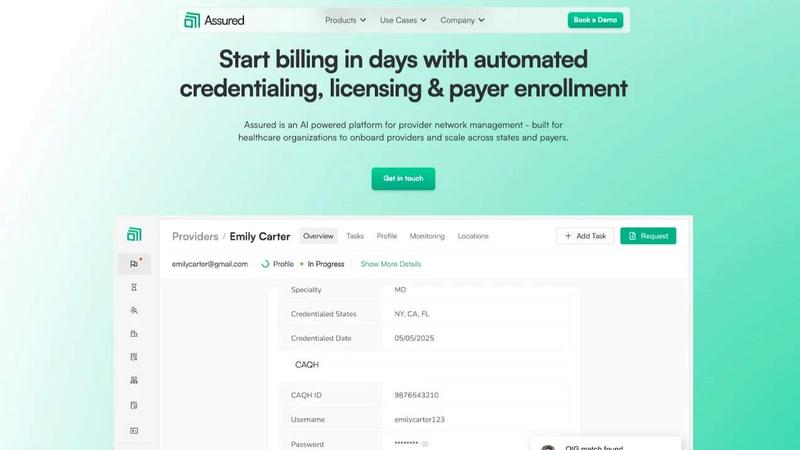
Overview
About AI Podcast Generator
AI Podcast Generator is an intelligent platform designed to simplify podcast creation using advanced AI voice and text processing technologies. Instead of recording, editing, and producing audio manually, users can simply input text, an article, or a topic idea, and the platform automatically generates a complete podcast episode with natural-sounding AI voices.
The platform is built for creators, marketers, educators, and storytellers who want to quickly produce professional podcast content without expensive equipment or complex editing software. AI Podcast Generator can convert blog posts, scripts, news summaries, educational materials, or storytelling ideas into engaging audio content within minutes.
With high-quality voice synthesis, multiple speaking styles, and fast audio generation, the platform enables users to create podcasts for content marketing, social media, learning materials, and media production. AI Podcast Generator helps transform written content into dynamic audio experiences, making podcast creation accessible to everyone.
About Assured
Assured is provider network management software that automates credentialing, payer enrollment, and provider network monitoring for healthcare organizations. Get providers credentialed in 48 hours instead of 60+ days. Get in-network 30% faster. Stop losing revenue to administrative backlogs.
Traditional credentialing vendors rely on offshore teams and manual data entry. Assured uses AI to verify credentials across 2,000+ primary sources in parallel, auto-generate applications, submit directly to payer portals, and flag sanctions within 24 hours. The platform is NCQA-certified as a Credentials Verification Organization (CVO).
The platform handles end-to-end credentialing, payer enrollment with automated roster management, and real-time provider network monitoring from 2,000+ data sources. Credential renewals initiate automatically 60 days before expiration. Sanctions detected 22 days earlier than manual processes. Payer enrollments achieve 95% first-pass approval rates. Integrates with
