Assured vs incentX
Side-by-side comparison to help you choose the right AI tool.
Assured
Assured uses AI to automate provider credentialing and enrollment so healthcare companies can start billing in days, not months.
Last updated: April 4, 2026
Automate your incentive compensation with precise data for accurate payouts and seamless performance alignment.
Last updated: March 1, 2026
Visual Comparison
Assured
incentX
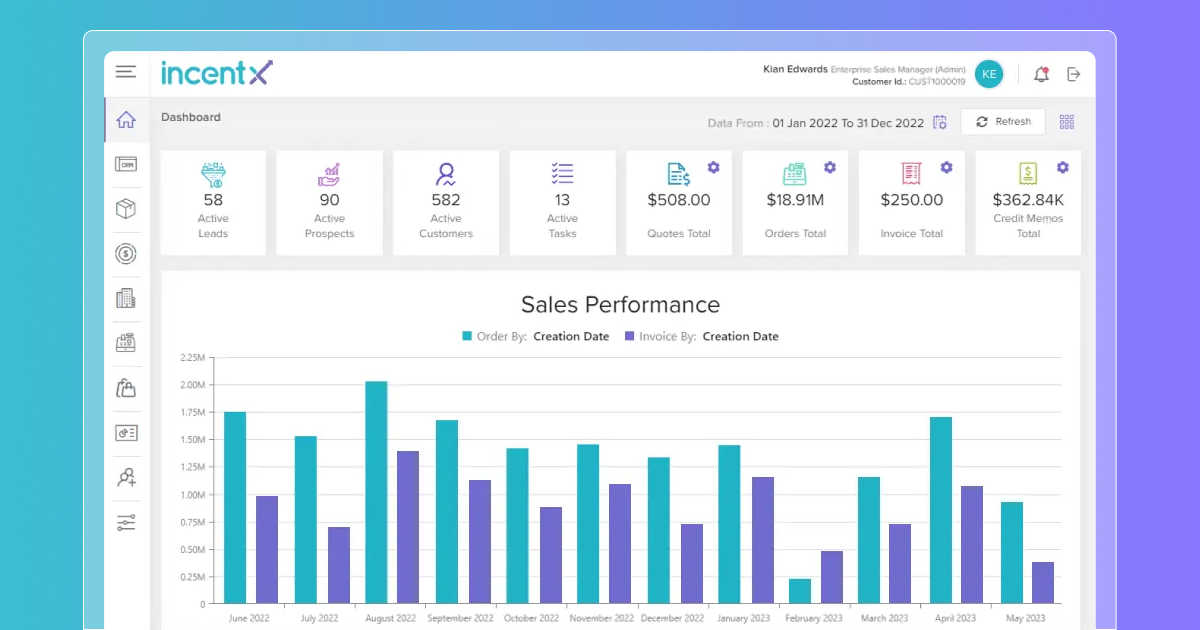
Feature Comparison
Assured
AI-Powered Primary Source Verification
Assured's AI engine automates the verification of provider credentials by checking over 2,000 primary sources simultaneously. This eliminates the slow, sequential manual checks that traditionally take weeks. The system instantly validates licenses, education, work history, and sanctions, flagging any issues within 24 hours to ensure compliance and dramatically accelerate the initial verification step.
Automated Payer Enrollment & Roster Management
This feature streamlines the entire payer enrollment process. Assured auto-generates completed applications specific to each payer's requirements and can submit them directly through payer portals. It also automates roster management, tracking submissions, follow-ups, and statuses in real time, which helps achieve a 95% first-pass approval rate and gets providers in-network 30% faster.
Proactive Credentialing & Licensing Renewals
Never let a credential expire again. Assured's platform proactively monitors all provider credentials and licenses, automatically initiating the renewal process 60 days before expiration. It handles submissions and follow-ups across all 50 states, removing the administrative chaos and risk associated with manual renewal tracking for multi-state organizations.
Real-Time Provider Network Monitoring
Gain a single, always-updated source of truth for your entire network. Assured continuously monitors your provider data against its 2,000+ verification sources, alerting you to any changes like new sanctions, license updates, or expirations. This ensures you're never surprised at audit time and can maintain a fully compliant, in-network provider roster.
incentX
Comprehensive Incentive Management
incentX offers a complete suite for managing various incentive programs such as rebates, royalties, trade promotions, and commissions from a single platform. This integration eliminates the need for multiple tools, ensuring accuracy and consistency across all compensation structures.
Transaction-Level Precision
With incentX, organizations can automate incentive calculations based on precise transaction data. This feature enhances accuracy and minimizes the risk of manual errors, allowing businesses to focus on strategic decisions rather than administrative tasks.
Real-Time Forecasting
The platform enables businesses to forecast payouts with unmatched accuracy. By linking commissions to fulfilled transactions rather than sales estimates, incentX helps eliminate commission overpayments and allows for precise budgeting based on actual margin and fulfillment data.
Visibility and Transparency
incentX provides stakeholders with real-time visibility into how each payout is calculated. This transparency reduces disputes and fosters trust among sales representatives, as they can see the transactions behind their earnings, leading to improved morale and performance.
Use Cases
Assured
Scaling a Digital Health Company Across States
For a digital health startup expanding its telehealth services, manually managing state-specific licensing and payer rules for new providers is a massive barrier. Assured automates multi-state licensure and payer enrollment, allowing the company to onboard providers uniformly and get them seeing patients in new states within weeks instead of months, enabling rapid, compliant growth.
Eliminating Credentialing Backlogs for Health Systems
Large health systems often face crippling backlogs where new hires wait 60+ days to be credentialed, delaying patient care and revenue. Assured's automated, end-to-end credentialing cuts this to days, clearing backlogs, accelerating time-to-revenue, and freeing up dozens of administrative hours per week for strategic work.
Ensuring Continuous Compliance for Provider Groups
Provider groups need to ensure every clinician remains in good standing with multiple payers and state boards. Manually checking for sanctions or expiring licenses is error-prone. Assured provides real-time monitoring and alerts, flagging issues 22 days earlier on average, which protects revenue and prevents compliance violations before they happen.
Streamlining Payer Enrollment for Specialized Clinics
A specialty clinic adding new physicians faces complex, payer-specific enrollment forms and slow follow-up processes. Assured automates application completion and submission, then actively tracks each enrollment through to approval. This results in a 95% first-pass rate, getting specialized care in-network faster so patients can access vital treatments without delay.
incentX
Sales Compensation Management
incentX is ideal for organizations looking to automate their sales compensation processes. By leveraging actual ERP transactions, businesses can align their sales goals with real revenue and margin data, ensuring fair and accurate payouts.
Rebate Program Optimization
Companies can streamline their rebate programs using incentX's real-time order and claim data. This feature eliminates shadow accounting practices, maximizing ROI by ensuring that rebates are accurately calculated and paid out based on actual performance.
Royalty Calculations
For organizations that rely on royalties, incentX enables calculations from real sales data rather than estimates. This ensures accuracy and compliance with audit requirements, allowing businesses to maintain trust with their partners and stakeholders.
Chargeback Management
incentX simplifies vendor chargeback processes by matching every deduction to transactions and returns. With full invoice-level visibility, businesses can effectively manage chargebacks and maintain accurate financial records, reducing disputes and improving operational efficiency.
Overview
About Assured
Assured is an AI-powered provider network management platform built to help healthcare organizations scale efficiently and stop losing revenue to administrative delays. It automates the complex, manual processes of credentialing, licensing, payer enrollment, and ongoing network monitoring. Designed for provider groups, health systems, payers, and digital health companies, Assured tackles the core problem of disconnected data and slow, error-prone manual work. Its core value proposition is dramatic speed and accuracy: get providers credentialed in 48 hours instead of 60+ days, achieve 95% first-pass approval rates for payer enrollments, and detect sanctions 22 days earlier than manual methods. As an NCQA-certified Credentials Verification Organization (CVO), Assured leverages AI to verify credentials across 2,000+ primary sources in parallel, auto-generate applications, and submit directly to payer portals. This means faster provider onboarding, quicker revenue generation, and complete peace of mind with real-time data monitoring, all from a single, centralized platform.
About incentX
incentX is an innovative incentive automation platform that revolutionizes how businesses manage their compensation processes. Tailored for revenue, finance, and operations teams, it streamlines various compensation structures, such as sales commissions, partner rebates, and royalties, all from a centralized source. By integrating seamlessly with your existing CRM and ERP systems, incentX ensures transaction-level calculations that eliminate the inefficiencies of manual spreadsheets and significantly reduce disputes. The platform empowers organizations with real-time visibility into payouts, enabling accurate compensation based on actual performance. This means companies can create realistic and impactful incentive plans that align directly with revenue generation. With incentX, businesses can eliminate manual processes, reduce IT dependencies, and ensure that every compensation structure is tied to measurable outcomes, driving profitable growth and operational efficiency.
Frequently Asked Questions
Assured FAQ
How does Assured reduce provider onboarding time and administrative costs?
Traditional credentialing is a manual, sequential process that takes 60+ days. Assured uses AI to perform verifications across thousands of sources in parallel and automates application submissions, reducing credentialing to about 48 hours. This efficiency saves organizations an estimated $4,200 to $5,800 in administrative costs per provider annually by eliminating manual labor and accelerating revenue-generating patient visits.
What makes Assured more reliable than traditional credentialing vendors?
Traditional vendors often rely on offshore teams and manual data entry, which can be slow and error-prone. Assured is an NCQA-certified CVO that uses AI for accuracy and speed, provides real-time data from primary sources, and offers full transparency within the platform. Its automated systems achieve a 95% first-pass approval rate for enrollments and detect issues far earlier, providing greater reliability and compliance confidence.
Can Assured integrate with our existing systems like our EMR or ATS?
Yes, absolutely. Assured is built with connectivity in mind. It offers plug-and-play APIs that allow you to seamlessly connect the platform to your existing Applicant Tracking System (ATS), Electronic Medical Record (EMR), or CRM like Salesforce. This ensures data flows smoothly between systems, eliminating duplicate data entry and creating a unified workflow.
How does the real-time network monitoring work?
Assured continuously scans its database of over 2,000 primary sources, including state medical boards, sanction lists, and payer rosters. It automatically compares this live data against your provider roster. If any change is detected—such as a new sanction, license update, or expiration—the platform immediately alerts your team, allowing for proactive management long before an audit or billing issue occurs.
incentX FAQ
What types of compensation structures can incentX manage?
incentX can manage a variety of compensation structures including sales commissions, partner rebates, royalties, chargebacks, and trade promotions, all integrated into one platform.
How does incentX ensure accuracy in incentive calculations?
By utilizing transaction-level data linked directly to ERP systems, incentX eliminates manual errors associated with spreadsheets, providing precise and accurate incentive calculations based on real performance metrics.
Can incentX integrate with my existing systems?
Yes, incentX is designed to seamlessly integrate with existing CRM and ERP systems, allowing for efficient data flow and real-time visibility into compensation processes without disrupting current workflows.
Is there a demo available for incentX?
Absolutely! incentX offers the opportunity to schedule a demo, allowing potential users to explore the platform's features and understand how it can benefit their specific compensation management needs.
Alternatives
Assured Alternatives
Assured is a specialized provider network management platform that automates credentialing and payer enrollment for healthcare organizations. It falls into the productivity and management software category, helping teams drastically reduce administrative backlogs and get providers to revenue faster. Users often explore alternatives for various reasons. Some may need a solution that integrates with a specific EHR or practice management system they already use. Others might be evaluating options based on budget constraints, looking for a different feature set, or requiring a platform that scales differently for a very large or very small organization. When choosing an alternative, it's crucial to consider a few key factors. Look for a platform's certification status, like NCQA-CVO, which is a gold standard for quality. Evaluate the depth of automation, especially for time-consuming tasks like primary source verification and payer application submission. Finally, consider the vendor's focus on security and compliance, as they will be handling sensitive provider data.
incentX Alternatives
incentX is a cutting-edge incentive automation platform that falls under the productivity and management category. It specializes in streamlining incentive compensation processes, such as sales commissions and partner rebates, through precise, transaction-level data. Organizations often seek alternatives to incentX due to various reasons, including cost considerations, specific feature requirements, or the need for better integration with existing systems. When searching for an alternative, it’s crucial to evaluate the platform's ability to manage diverse compensation structures, the accuracy of its forecasting capabilities, and how well it integrates with your current tools. Additionally, consider the level of automation offered and the transparency provided in payout calculations, as these elements can significantly impact overall efficiency and user satisfaction.

